2021-11-02
Mechanism deciphered: How the coronavirus damages blood vessels in the brain
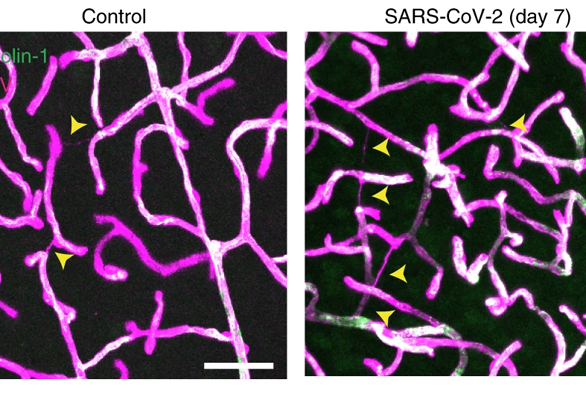
The brain accumulates dead blood vessels after Sars-CoV-2 infection (arrowheads, results from mice), Image from Wenzel et al., Nature Neuroscience (2021)
Sars-CoV-2 affects not only lungs and airways, but influences many organs of the human body. How it damages small blood vessels in the brain was deciphered by a consortium of the German Centers for Lung Research (DZL), Infection Research (DZIF) and Cardiovascular Research (DZHK). They published their results last week in Nature Neuroscience. Prof. Peter König of DZL site ARCN accounted for electron miscroscopy.
Sars-CoV-2 coronavirus enters the body via the respiratory tract and lungs and airways are the obvious center of the disease symptoms. However, it was shown early on that many other organs and the blood vessels are also affected. For example, neurological symptoms can occur in both the acute and late phases of the disease. These include frequent anosmia or epileptic seizures, strokes, loss of consciousness, and confusion. How coronavirus triggers these cognitive and psychiatric symptoms is largely unclear. Results are conflicting, if the coronavirus directly attacks brain cells. What is known, however, is that it attacks blood vessels – including those in the brain. Against this background, an international consortium led by the Lübeck pharmacologist Prof. Markus Schwaninger (DZHK) asked what mechanism underlies the brain damage. To this end, the group focused on the small blood vessels and the endothelial cells that line them.
How the coronavirus damages the brain
The study results show that the coronavirus can indeed enter the cell via the ACE2 receptor produced by some endothelial cells and trigger a characteristic pathology that can be seen under the microscope. In endothelial cells, the viral enzyme Mpro destroys the endogenous protein NEMO, triggering a cell death program. A key finding of the study is that endothelial cells and blood-brain barrier are destroyed in this way. The scientists thus discovered for the first time a mechanism by which Sars-CoV-2 directly damages microvessels in the brain.
Possible therapeutic pathways elucidated
Interestingly, the researchers found a way to block the cell death mechanism by investigating another protein involved in this process, RIPK1. If RIPK1 is blocked in animal experiments, the endothelial cells don’t die. The entire cell death program is thus deactivated – regardless of whether NEMO was cleaved by the viral enzyme Mpro or not. RIPK1-blocking compounds are already in the early stages of clinical testing. “The results of our study suggest that such drugs could alleviate neurological long covid symptoms,” says Markus Schwaninger.
Successful cooperation of several German Centers for Health Research (DZG)
For the study, researchers from the German Centers for Lung Research (DZL), Infection Research (DZIF) and Cardiovascular Research (DZHK) collaborated in an interdisciplinary manner. They used different animal models as well as samples from Covid-19 patients. An impressive number of different methodologies were used. Of particular note are microscopic techniques for visualizing the brain’s small blood vessels. “Without our high-resolution STED microscope*, imaging of brain vessels could not have been performed in this way,” explains Prof. Peter König (University of Lübeck) from the DZL site ARCN. He procured the device together with Prof. Gereon Hüttmann (also ARCN) and study head Schwaninger (DZHK) through the German Research Foundation (DFG). The results, which have now been published in Nature Neuroscience, demonstrate the importance of basic research as an impulse for the development of drugs, the so-called translation.
*STED microscope = STimulated Emission Depletion microscope
Original paper: Wenzel J, Lampe J, Müller-Fielitz H, Schuster R, Zille M, Müller K, Krohn M, Körbelin J, Zhang L, Özorhan Ü, Neve V, Wagner JUG, Bojkova D, Shumliakivska M, Jiang Y, Fähnrich A, Ott F, Sencio V, Robil C, Pfefferle S, Sauve F, Coêlho CFF, Franz J, Spiecker F, Lembrich B, Binder S, Feller N, König P, Busch H, Collin L, Villaseñor R, Jöhren O, Altmeppen HC, Pasparakis M, Dimmeler S, Cinatl J, Püschel K, Zelic M, Ofengeim D, Stadelmann C, Trottein F, Nogueiras R, Hilgenfeld R, Glatzel M, Prevot V, Schwaninger M (2021) The SARS-CoV-2 main protease Mpro causes microvascular brain pathology by cleaving NEMO in brain endothelial cells. Nat Neurosci 24: 1522-1533
Source: Link to Nature Neuroscience article
/jbul
Calendar
Upcoming events
2024-04-30
Virtual DZL AID Kick-off Seminar
2024-05-29
74th Meeting of ARCN
2024-06-05
